For decades, checking on cancer meant a needle, a scalpel, and a long wait. Doctors cut into tumors-sometimes deep in the lung, spine, or liver-to get tissue samples. But what if you could track cancer with just a simple blood draw? That’s the promise of liquid biopsy, and it’s no longer science fiction. It’s happening in clinics right now, especially for people with advanced cancer.
What Is Circulating Tumor DNA (ctDNA)?
Circulating tumor DNA, or ctDNA, is tiny fragments of DNA that cancer cells shed into the bloodstream. When a tumor cell dies, it breaks apart, and pieces of its genetic code float around in the blood like digital breadcrumbs. These fragments carry the same mutations that drive the cancer-whether it’s an EGFR change in lung cancer, a KRAS mutation in colorectal cancer, or a BRCA alteration in breast cancer.
Unlike a tissue biopsy that only samples one spot, ctDNA gives you a full picture. Tumors aren’t uniform. One part might be resistant to a drug, while another isn’t. A single biopsy might miss that. But ctDNA? It pulls genetic material from all those different regions. That’s why it’s so powerful for tracking how cancer evolves over time.
Why Liquid Biopsy Beats Traditional Biopsy
Traditional biopsies have real downsides. They’re invasive. They can cause bleeding, infection, or even collapse a lung. Some tumors are too risky or too hard to reach. And once you take the sample, you’re stuck with that snapshot in time. If the cancer changes, you need another surgery-and that’s not always possible.
Liquid biopsy changes all that. It’s a needle in the arm. No anesthesia. No recovery. You can do it every few weeks. That means doctors can see if a treatment is working before an MRI shows any change. In fact, studies show ctDNA can detect cancer returning six to eleven months before imaging does. That’s huge. It gives patients a chance to switch therapies before the disease spreads further.
For patients with metastatic cancer, liquid biopsy has cut the need for repeat tissue biopsies by 25-30%. That’s not just comfort-it’s safety. And for those whose tumors are too small or too fragile to biopsy, it’s often the only way to get molecular data.
How It Works: From Blood to Answers
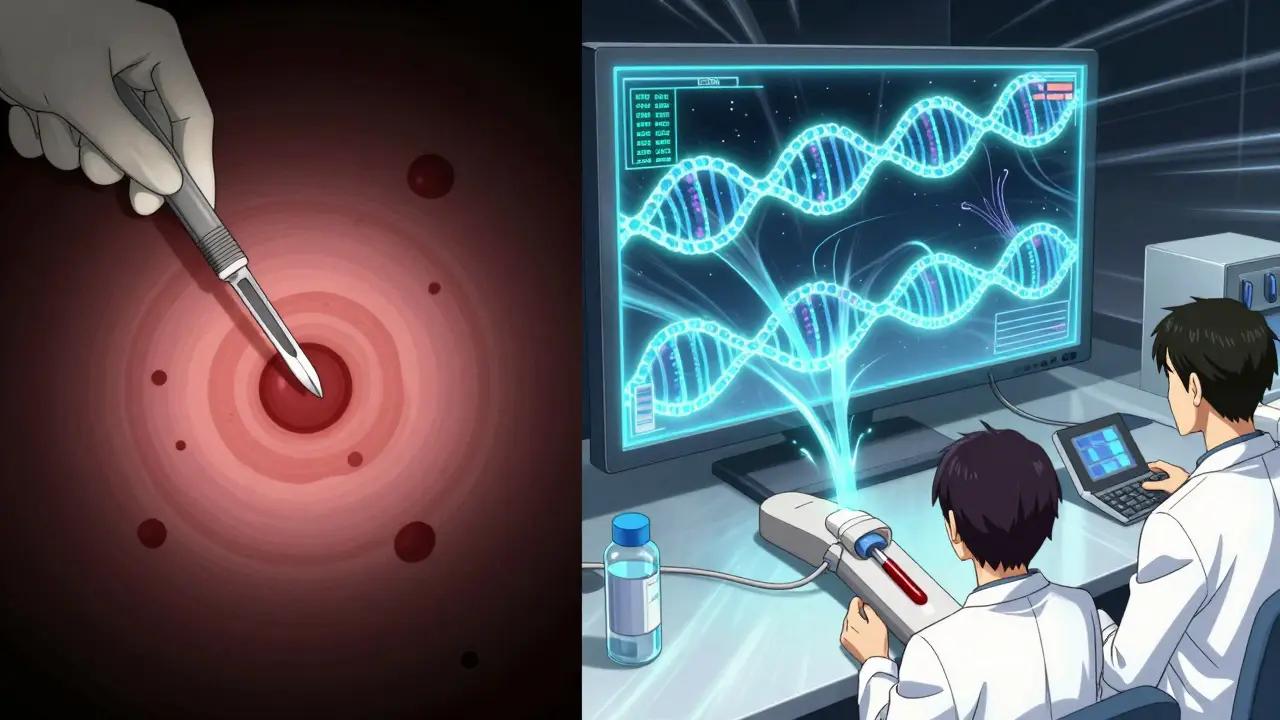
Here’s how it actually happens in a lab. A vial of blood is drawn. The plasma is separated from the cells. Then, scientists isolate the free-floating DNA. Most of it comes from healthy cells. But they’re looking for the rare cancer signals-maybe one mutated piece in 10,000 normal ones.
To find those needles, they use tools like digital droplet PCR (ddPCR) and next-generation sequencing (NGS). ddPCR can count exact numbers of mutant DNA molecules. NGS scans hundreds of genes at once. Some newer methods even look at how the DNA fragments are shaped-cancer DNA tends to break in specific patterns. Others check methylation-the chemical tags that turn genes on and off. In fact, combining methylation patterns with ctDNA can boost detection rates by 20-30%.
There are two main approaches: tumor-informed and tumor-agnostic. Tumor-informed means you first sequence the original tumor tissue, then build a custom test to look for those exact mutations in the blood. It’s super sensitive. Tumor-agnostic uses a broad panel to scan for common cancer mutations without needing prior tissue. It’s faster, but might miss rare changes.
Where It’s Making the Biggest Difference
Not all cancers are equal when it comes to ctDNA. Some shed DNA like crazy. Others barely leak any.
Lung cancer: This is where liquid biopsy shines. For non-small cell lung cancer, guidelines now say if tissue isn’t available, use a blood test to check for EGFR, ALK, or ROS1 mutations. In one study, ctDNA found targetable mutations in 92% of cases where tissue failed.
Colorectal cancer: ctDNA is used to check for recurrence after surgery. If it’s detectable three months post-op, the chance of relapse jumps to over 80%. That means doctors can start chemo early-or avoid it if ctDNA stays clear.
Breast cancer: Monitoring for resistance mutations like ESR1 helps switch from hormone therapy to newer drugs before tumors grow.
Prostate cancer: Not as strong. These tumors shed less DNA. But for advanced cases, ctDNA helps track AR-V7 mutations that signal resistance to common drugs.
For brain tumors? Still tricky. The blood-brain barrier blocks most DNA from escaping. Same with some slow-growing blood cancers. Liquid biopsy isn’t magic-it has limits.
The Real-World Challenges
Even with all this promise, there are roadblocks.
Early-stage cancers: Only 50-70% of stage I tumors release enough ctDNA to be detected. That’s why it’s not yet used for screening healthy people. But research is closing that gap fast.
False signals: Not every mutation in the blood comes from cancer. As people age, blood cells can pick up random mutations-called clonal hematopoiesis. These show up in 10-15% of people over 65. Labs now use special filters to spot these imposters, but it’s not foolproof.
Unknown variants: About 15-20% of reports show mutations with unclear meaning. Is it driving the cancer? Or just noise? That’s where doctors need experience-and sometimes, a tissue biopsy to confirm.
Standardization: Different labs use different machines, different blood tubes, different processing times. One study found up to 25% of results varied between centers. That’s why guidelines now stress using certified labs and following strict protocols.
What’s Next? The Future of ctDNA
The next five years will change everything.
Multi-analyte tests are coming-combining ctDNA, methylation, fragment patterns, and even RNA fragments. Early data suggests this could push early-detection sensitivity past 95%. Imagine a blood test that finds five types of cancer before symptoms appear.
AI is jumping in too. Researchers at MD Anderson are training algorithms to read the shape of DNA fragments. Cancer DNA breaks differently than healthy DNA. AI can spot those patterns better than humans. Early results show a 15-20% boost in accuracy.
And regulatory approval? The FDA has approved 12 liquid biopsy tests since 2020. Companies like Guardant360 and FoundationOne Liquid CDx are now standard tools in oncology.
More than 60-70% of academic cancer centers offer liquid biopsy. Community clinics are catching up, though cost and interpretation training are still barriers.
Is It Right for You?
If you have advanced cancer-especially lung, colorectal, or breast cancer-and are on targeted therapy, liquid biopsy is likely already part of your care. It helps answer: Is the drug working? Is resistance building? Should we switch?
If you’re in early-stage cancer, it’s mostly used after surgery to check for minimal residual disease. If ctDNA is gone, you might avoid chemo. If it’s still there, you get treatment early.
It’s not for everyone. For low-shedding cancers, it’s less useful. For screening healthy people? Still not ready. But for monitoring? It’s becoming essential.
One thing’s clear: cancer care is shifting from fixed snapshots to continuous movies. And ctDNA is the camera.
Can liquid biopsy replace tissue biopsy completely?
No-not yet. Tissue biopsy is still needed for initial diagnosis, especially to confirm cancer type and grade. Liquid biopsy is best for monitoring after diagnosis. It’s a complement, not a replacement.
How often should ctDNA be tested during treatment?
During active treatment, every 4-8 weeks is typical. For surveillance after therapy, every 3-6 months. But it depends on the cancer type and treatment. For example, lung cancer patients on targeted therapy often get tested monthly to catch resistance early.
Can liquid biopsy detect cancer before symptoms appear?
Not reliably yet. For stage I cancers, detection rates are still only 50-70%. Research is improving this, especially with methylation and AI, but it’s not ready for population-wide screening. It’s currently used for high-risk individuals or those with known cancer.
What if the liquid biopsy result is negative but I still have symptoms?
A negative result doesn’t rule out cancer. Some tumors shed very little DNA. If symptoms persist, imaging or tissue biopsy may still be needed. Liquid biopsy is one tool-not the whole toolkit.
Is liquid biopsy covered by insurance?
In many cases, yes-especially for advanced non-small cell lung cancer, colorectal cancer, and breast cancer when tissue is insufficient. Medicare and most private insurers cover FDA-approved tests like Guardant360 CDx and FoundationOne Liquid CDx. Always check with your provider and oncologist.


Korn Deno
March 24, 2026 AT 15:30Aaron Sims
March 25, 2026 AT 21:31peter vencken
March 26, 2026 AT 19:27Rama Rish
March 26, 2026 AT 22:47Jesse Hall
March 27, 2026 AT 22:55Donna Fogelsong
March 28, 2026 AT 12:50Sean Bechtelheimer
March 29, 2026 AT 20:55Seth Eugenne
March 30, 2026 AT 01:30Caroline Dennis
March 30, 2026 AT 22:36