Imagine waking up and feeling like your body's internal engine has simply run out of fuel. You're exhausted, your muscles are aching, and you have a strange craving for salty snacks. For someone with Addison's Disease is a chronic endocrine disorder where the adrenal glands fail to produce enough essential hormones, specifically cortisol and aldosterone. It isn't just a feeling of fatigue; it's a systemic failure that can become life-threatening in a matter of hours if not managed correctly. The challenge is that most people don't realize they have it until about 90% of their adrenal function is gone, making the diagnosis a sudden and often frightening wake-up call.
Quick Facts on Adrenal Insufficiency
- The Cause: In developed countries, 80-90% of cases are autoimmune, meaning the body attacks its own adrenal cortex.
- Key Deficiencies: Lack of cortisol (the stress hormone) and aldosterone (the salt-regulating hormone).
- The Danger: An "adrenal crisis" can cause a sudden drop in blood pressure and shock.
- The Fix: Lifelong hormone replacement therapy to mimic the body's natural rhythms.
What Exactly Is Happening in the Body?
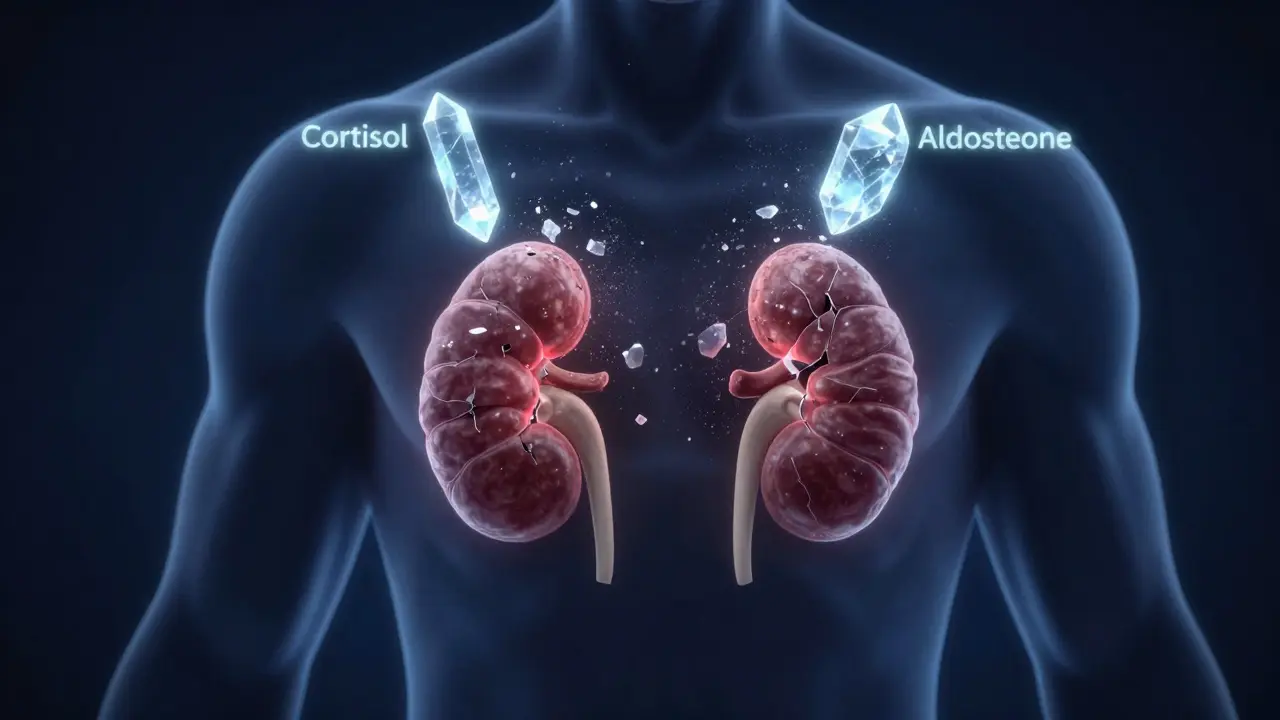
To understand this condition, you have to look at the adrenal glands-two small hats sitting on top of your kidneys. These glands produce hormones that keep you alive. When you have Addison's, the adrenal cortex is destroyed. This is often tracked by the presence of 21-hydroxylase antibodies, which act as the smoking gun for an autoimmune attack.
The two missing pieces of the puzzle are cortisol and aldosterone. Cortisol is your body's primary stress responder; it helps regulate blood sugar and manages inflammation. Aldosterone acts like a salt-manager, telling your kidneys to hold onto sodium and release potassium. Without them, your blood pressure plummets, and your electrolytes go haywire. You might notice hyperpigmentation-a darkening of the skin, especially on knuckles or scars-because the pituitary gland pumps out massive amounts of ACTH to try and wake up the dormant adrenal glands, which accidentally stimulates pigment-producing cells in the skin.
Primary vs. Secondary Adrenal Insufficiency
Not all adrenal failure is the same. While we often use the terms interchangeably, there is a massive difference between primary and secondary versions. In primary insufficiency (classic Addison's), the problem is in the glands themselves. In secondary insufficiency, the glands are fine, but the Pituitary Gland isn't sending the signal to start production.
| Feature | Primary (Addison's) | Secondary |
|---|---|---|
| Cause | Adrenal gland destruction | Pituitary/Hypothalamus failure |
| Aldosterone | Deficient (Low) | Usually Normal |
| Skin Color | Hyperpigmentation (Darkening) | No change/Pale |
| Electrolytes | High Potassium / Low Sodium | Generally Normal |
| Treatment | Glucocorticoids & Mineralocorticoids | Glucocorticoids only |
The Roadmap to Diagnosis
Getting a diagnosis isn't always a straight line. Many patients spend over three years visiting general practitioners or gastroenterologists because their symptoms-like nausea and weight loss-look like common stomach bugs. The gold standard for confirmation is the ACTH stimulation test (or cosyntropin test). During this test, a doctor gives you a synthetic version of the hormone that triggers cortisol production. If your cortisol levels don't rise above 18 mcg/dL within an hour, the diagnosis is confirmed.
Beyond the cortisol check, doctors look for salt imbalances. A classic sign is hyponatremia (low sodium) and hyperkalemia (high potassium). Because this is often an autoimmune issue, it rarely travels alone. Roughly half of people with Addison's will develop other autoimmune conditions, such as type 1 diabetes or autoimmune thyroid disease. It's a package deal that requires a vigilant endocrinologist to monitor annually.
Mastering Steroid Replacement Therapy
Since your body can no longer make these hormones, you have to put them back in manually. This isn't a one-pill-a-day situation for most; it's about mimicking a biological clock. Hydrocortisone is the standard glucocorticoid used to replace cortisol. Most people take it in divided doses-a larger dose in the morning and a smaller one in the afternoon-to reflect how a healthy body naturally releases cortisol.
If you have primary adrenal insufficiency, you also need Fludrocortisone. This mineralocorticoid replaces aldosterone, keeping your blood pressure stable and preventing your body from wasting salt. This is where the balancing act becomes critical. Over-replacing these steroids can lead to cardiovascular issues, while under-replacing them puts you at a massive risk for a crisis. It's a narrow window that requires precise dosing and a lot of patient-doctor communication.
The Danger Zone: Preventing Adrenal Crisis
An adrenal crisis is the nightmare scenario for any patient. It happens when the body is under stress-like during a severe infection, a car accident, or even a high fever-and cannot produce the extra cortisol needed to cope. Without a dose increase, your blood pressure can crash, leading to shock and coma.
This is why "Sick Day Rules" are non-negotiable. If you're vomiting and can't keep your pills down, you can't just wait it out. You need an emergency injection of hydrocortisone. The difference in survival is stark: patients who carry emergency kits and wear medical alert bracelets have significantly lower mortality rates. If you're headed for a dental procedure or a minor surgery, you'll need "stress dosing," which might involve an IV of hydrocortisone to keep your system stable while the body is under pressure.
Living with the Condition in 2026
The landscape of treatment is evolving. For a long time, the struggle was the "rollercoaster" effect of immediate-release tablets. However, newer options like modified-release hydrocortisone aim to provide a more steady, physiological release of the hormone, reducing the wild fluctuations that leave patients feeling wired one hour and crashed the next.
The psychological toll is real. The constant fear of a crisis during a simple flu can be exhausting. But there is a light at the end of the tunnel. Emerging technology, including continuous cortisol monitoring devices, is moving toward a future where your medication could potentially adjust itself in real-time, much like a continuous glucose monitor does for diabetics. Until then, education is your best defense. Learning how to adjust your dose at 3:00 AM when a fever hits is the most valuable skill you can acquire.
Can Addison's disease be cured?
No, there is no cure for the autoimmune destruction of the adrenal glands. However, it is highly manageable with lifelong hormone replacement therapy. With the correct dose of glucocorticoids and mineralocorticoids, most people live a full and active life.
What are the "Sick Day Rules"?
Sick day rules are a set of protocols to prevent adrenal crisis. They typically include doubling or tripling your oral hydrocortisone dose during a fever or illness. If you are vomiting or unable to swallow, the rule is to immediately administer an emergency intramuscular or intravenous injection of hydrocortisone.
Why do I crave salt with Addison's?
The lack of aldosterone causes your kidneys to dump sodium into your urine rather than keeping it in your blood. This creates a biological drive to consume more salt to maintain blood pressure and electrolyte balance.
Is it possible to misdiagnose Addison's?
Yes, it is very common. Because the symptoms are vague-fatigue, nausea, weight loss-it is often mistaken for depression, chronic fatigue syndrome, or gastrointestinal issues. Some patients are misdiagnosed for over three years before an ACTH stimulation test is performed.
What happens if I miss a dose of my steroids?
Missing a single dose might only cause mild fatigue, but missing multiple doses or skipping them during a stressful event can trigger an adrenal crisis. This is why consistency is vital and why a medical alert ID is recommended.
Next Steps and Support
If you suspect you have adrenal insufficiency, your first stop should be an endocrinologist. Don't rely on a standard blood test; ask specifically about the ACTH stimulation test. If you've already been diagnosed, focus on three things: get a medical alert bracelet, set up an emergency injection kit, and memorize your sick day rules. Joining a support group, such as the Addison's Disease Self Help Group, can also help you navigate the nuances of dose adjustments that textbooks often overlook.


Doug DeMarco
April 11, 2026 AT 03:50Spot on info! Always remember to keep your emergency kit in a place where anyone can find it, not just tucked away in a drawer! 💊✨ Stay safe everyone!
Chad Miller
April 11, 2026 AT 14:25most ppl just dont read the labels anymore and expect a doctor to fix everything without doing the legwork its just sad
Robin Walton
April 12, 2026 AT 06:16It's so frightening to think how long some people go without a diagnosis. I really hope anyone feeling these symptoms finds a doctor who actually listens to them.
Camille Sebello
April 13, 2026 AT 18:51Need your blood type!!! Which clinic did you use???
Julie Bella
April 14, 2026 AT 16:59Honestley you should be sharing your whole med history here so we can all help!! Its just common sense to be open about health!!! :)
Simon Stockdale
April 16, 2026 AT 00:55This is why we need real American medicine and not some fancy globalist nonsense they probably want us on these meds forever just to keep us weak while the real patriots are out there actually fighting for this country and making sure we dont get tricked by some big pharma scheme that probably started in a lab across the ocean and now they want us to pay for it with our own taxes which is just plain wrong if you ask me!!
Will Gray
April 17, 2026 AT 04:22Notice how the 'gold standard' test is just another way for the medical establishment to gatekeep diagnosis. It's a curated system designed to maintain a dependency on synthetic hormones while the true cause of adrenal failure is likely masked by environmental toxins they refuse to acknowledge.
Rakesh Tiwari
April 18, 2026 AT 14:39Oh, look at us, relying on 'synthetic versions' of hormones. How absolutely revolutionary. I'm sure the pharmacological industry is just heartbroken by your struggle.
Suchita Jain
April 19, 2026 AT 21:15It is quite evident that many individuals lack the discipline to maintain a strict hormonal regimen. One must approach their biological equilibrium with utmost gravity and adherence to the prescribed protocols.
emmanuel okafor
April 20, 2026 AT 04:55we all just want to be healthy and live in peace with our bodies
Danny Wilks
April 21, 2026 AT 11:05I find it quite fascinating how the biological drive for salt manifests as a psychological craving, almost as if the mind is attempting to bridge the gap created by the endocrine system's failure through behavioral adaptation, which is a nuance often overlooked in the sterile environments of modern clinical settings where the human experience is secondary to the data point.
Sarina Montano
April 22, 2026 AT 08:15The metabolic symphony of the adrenal glands is truly a precarious balance, and the introduction of modified-release hydrocortisone is a shimmering beacon of hope for those tired of the cortisol rollercoaster. It is an intricate dance of biochemistry where a few milligrams can be the difference between a vibrant day and a crushing fog, making the quest for physiological mimicry an absolute necessity for the long-term vitality of the patient. This evolution in delivery systems effectively smooths out the peaks and valleys that have historically plagued replacement therapy, allowing for a more seamless integration into a patient's daily life. We are finally seeing the shift from blunt-force dosing to a more nuanced, rhythmic approach that respects the body's inherent circadian patterns. This leap forward is not merely an improvement in convenience but a fundamental upgrade in the quality of life for thousands who have spent years navigating the precarious edge of an adrenal crisis. The psychological relief of knowing that your levels aren't plummeting the moment you step away from your pill bottle is immeasurable. It transforms the disease from a constant, looming threat into a manageable backdrop of one's existence. Furthermore, the synergy between mineralocorticoid stability and glucocorticoid rhythm is where the true magic of health happens. When the salt-water balance is locked in, the brain can finally stop screaming for sodium, and the body can focus on healing. This holistic stabilization is the real goal of modern endocrinology. It is a beautiful intersection of chemistry and care that allows a person to reclaim their autonomy from a failing gland. I am genuinely thrilled by the trajectory of these pharmacological advancements. The future of endocrine management is looking increasingly bright, moving us closer to a world where chronic illness is a footnote rather than a headline. It is a testament to human ingenuity and the persistent drive to refine our understanding of the inner workings of the human machine. Let us hope these advancements reach every corner of the globe soon.